Maternal health refers to the health of women during pregnancy, childbirth, and the postnatal period. It is influential in determining the overall health outcomes of both mother and baby, making a woman’s preconception health and ability to access maternal healthcare extremely important. Prenatal care is critical as it allows expecting mothers to be screened and monitored for potential complications that could occur during and after pregnancy. Access to prenatal care reduces the risk of many pregnancy complications that can be dangerous and even fatal for both the mother and baby, especially if left undiagnosed.
While genetics can play a role in maternal and infant health outcomes, the preconception health of a mother is critical. Research strongly supports that where people live, learn, work, and play (in addition to environmental and social factors and availability of resources to meet daily needs) influence maternal and infant health behaviors and health status.
Pregnant women living in rural communities face unprecedented barriers to accessing adequate maternity care, often leading to disparate birth outcomes. Rural women often face lengthy journeys to reach a hospital that offers obstetric care. The scarcity of obstetricians practicing in rural areas increases the number of births without obstetrician care and influences the number of early elective deliveries through the induction of labor and cesarean section procedures. The complications associated with these procedures present increased risks of maternal and infant mortality. The likelihood of facing these challenges is even greater for women of color in rural areas as they are disproportionately affected by a lack of access to maternal care and have a higher incidence of maternal mortality.
In Virginia, rural communities have a higher rate of infants born with low birth weight.
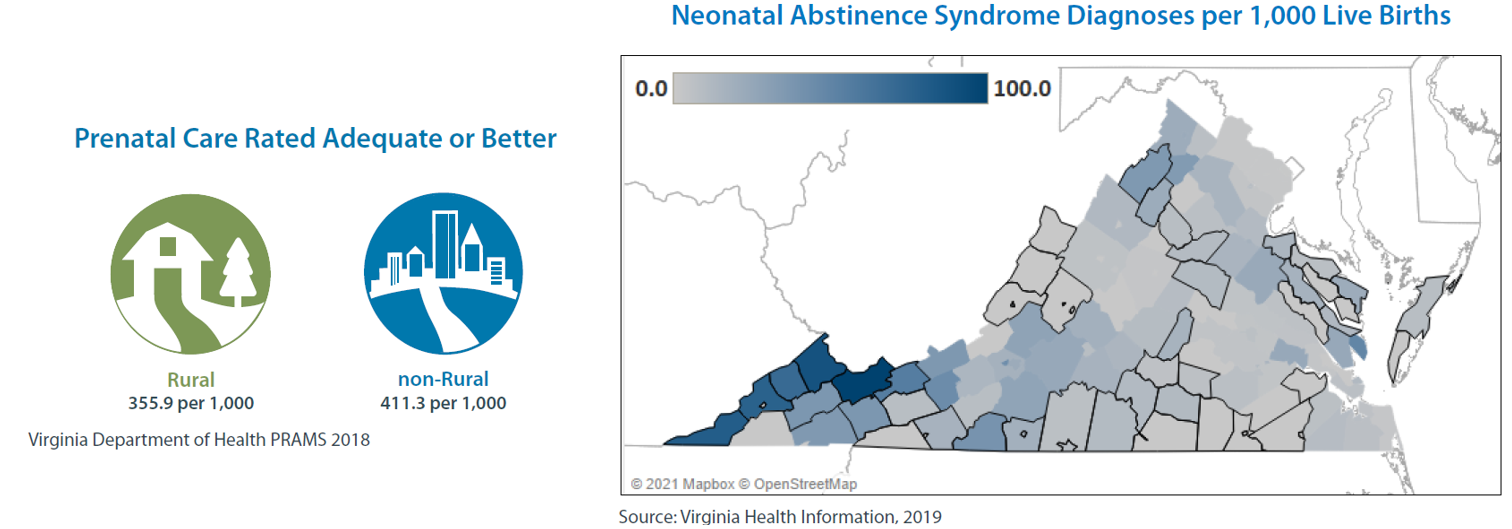
In rural areas, the rate of low birth weight is approximately 94 per 1,000 live births, compared to 82 per 1,000 in non-rural areas. However, there is much variation regionally. In Eastern Virginia, there are 123 babies born annually with low birth weight per 1,000 live births. In Northern Virginia, that number falls to 72. Additionally, low birth weight is often seen in babies with Neonatal Abstinence Syndrome (NAS), which occurs more frequently in rural areas.
Time between births is a concern for rural mothers and babies.
Children in rural areas are born with a birth interval of less than two years at over twice the rate of non-rural area; 190 per 1,000 live births in rural areas compared to just 89 per 1,000 live births in non-rural areas. Short birth rate intervals increase the risk of the mother not recovering fully from previous births, creating a sub-optimal environment for the next baby. These conditions can cause complications such as low birth weight and higher mortality rates in future births.

