Access to healthcare refers to both the availability and obtainability of health care services. Health care services include, but are not limited to: primary care, dental care, behavioral health, specialty care, emergency care, and public health services. Simply put, access to healthcare means that everyone has the ability to find the type of health care service(s) that they need, when they need it, and are able to pay for those services. This includes ancillary care and access to physical, respiratory, cardiovascular, and pulmonary therapies that prolong and enhance life and keep populations healthy. Access to healthcare is important for a person’s overall physical, social, and mental health status, disease prevention, detection, diagnosis, treatment of illnesses, and quality of life.
Generally speaking, the reasons people are unable to access healthcare when they need it are due to an inability to find an appropriate provider or insufficient resources to afford the care needed. Additional barriers include the inability to take time off work for an appointment, inadequate access to transportation to travel to the appointment, and limited options to improve health literacy of the patients.
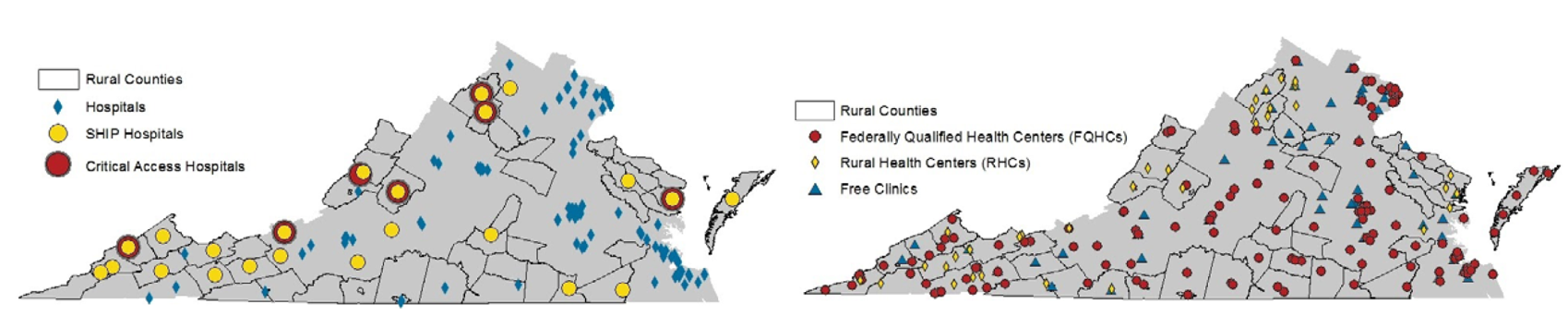
Many of Virginia’s rural areas are federally designated Health Professional Shortage Areas (HPSAs), for dental health, mental health and primary care. This definition means the area lacks enough providers for the population. Other communities might have providers but they may not accept the patient’s insurance plan. Some communities lack ancillary or specialty providers. Many rural counties lack a hospital and some of these communities rely heavily on volunteer emergency medical service providers.
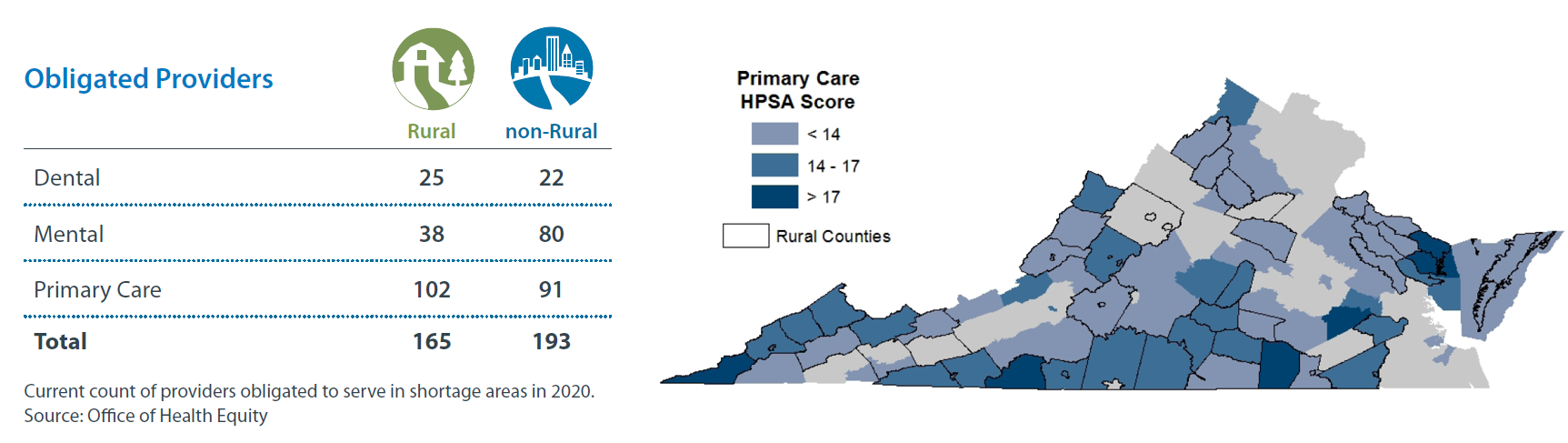
The VA-SORH team held a series of conversations with several rural communities across the Commonwealth. During these community conversations, access to healthcare services was unanimously identified as an issue or barrier community members faced which inhibited their ability to achieve optimal health and well-being. The issue was particularly notable in Lee County (Pennington Gap) and Patrick County (Stuart), where both communities had recently lost their rural hospitals. In Patrick County, EMS personnel reported routinely transporting patients two hours to North Carolina or Roanoke, keeping the ambulance out of service for up to 4 hours. Communities on the Eastern Shore have a robust clinical system available but most specialty care is across the Chesapeake Bay Bridge-Tunnel, which spans 17.6 miles with an eighteen dollar toll each way.
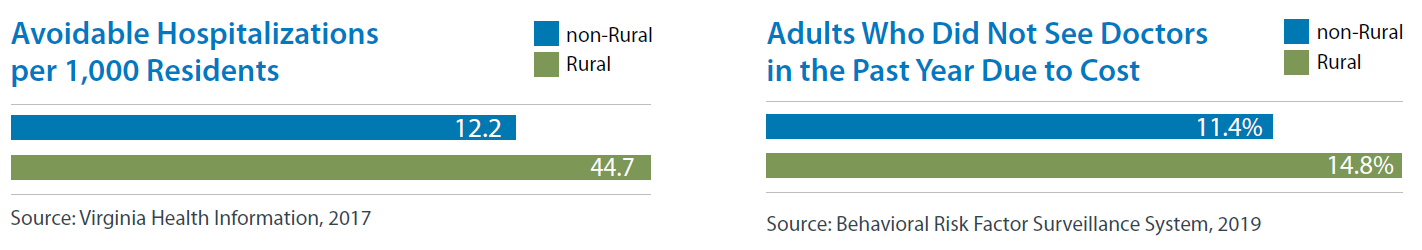
One way to measure access to care and its impact is to examine the number of avoidable hospitalizations. These are hospitalizations that could have been prevented if adequate care was available outside of the hospital setting, as defined by the US Agency for Healthcare Research and Quality (AHRQ). In 2017 throughout rural Virginia, there were about 20.6 avoidable hospitalizations per 1,000 residents compared to just 12.2 for non-rural residents. Avoidable hospitalizations per 1,000 residents are particularly low in Northern Virginia, just 6.8 per 1,000 residents. While the age and health of these populations is one factor driving per capita numbers, these factors demonstrate the need for improved access to primary care and other outpatient services in rural communities.
